Why you might need to see a varicose veins doctor, Singapore Vascular & Interventional Centre.
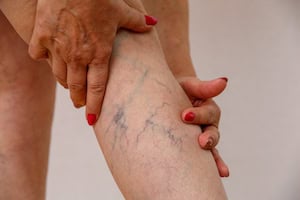
Taken from University of Utah Health.
What are Varicose Veins?
Varicose veins (Singapore) are blue or purple bulging, twisted veins which are mostly found on the lower body (legs and feet). They are usually not serious, but it is possible for them to cause pain and significant discomfort when inflamed or thrombosed. A milder version of varicose veins are spider veins, which are red, thinner veins found on the face and legs.
Veins are responsible for transporting blood from the rest of the body to the heart, which means the blood in your leg veins and the lower half of your body has to travel against gravity to reach its destination. When the muscles in our legs contract, the contractions help pump the blood upwards. The valves in the veins open to allow the blood to flow towards the heart and close to prevent the blood from flowing back downwards (backflow or reflux). But if the valves are damaged or weakened, they will not be able to close properly and stop all the blood in the veins from flowing towards the legs. Faulty valves cause blood to pool in the veins in the legs, resulting in swelling or enlargement of the veins thus leading to varicose veins. [1]
Here are a few risk factors for developing varicose veins:
- Age
- As you get older, the valves in your veins become weaker due to wear and tear, hence it becomes easier for blood to collect in your legs and form varicose veins.
- Family history
- If your immediate family members have or previously had varicose veins, you are more likely to have them as well.
- Abnormal hormonal changes
- Progesterone is a hormone produced in high quantities during pregnancy. It has the effect of dilating (widening) blood vessels. The vein wall is especially sensitive to the effects of Progesterone and high levels of this hormone can weaken the vein wall and damage the valves leading to the development of varicose veins.
- Pregnancy
- The growing weight of a baby increases the pressure on the veins in your lower body, hence causing more blood to pool in the veins instead of flowing to the heart. Varicose veins caused by pregnancy may go away after three months to a year, or may persist if there is permanent damage to the valves in the vein.
- Inactivity for long periods of time
- When you stand or sit down for a long time, your legs don’t move enough for your blood to circulate effectively. This increases the likelihood of blood collecting in the veins in your legs and feet resulting in stretching of the vein wall and subsequent valve damage leading to varicose veins.
If I have varicose veins (Singapore), what should I do? (treatment)
If varicose veins do not affect your daily life to a significant extent, and does not cause you much pain, home treatment should be sufficient. Home treatment comprises:
- Physical activity
- Exercise improves blood circulation, as blood has to flow in and out of the heart at a faster rate in order to transport enough oxygen to the muscles.
- Regularly doing light exercise such as walking, stretching and swimming is good as it poses less risk of physical injury while circulating the blood in the calf muscles. [3]
- Compression stockings
- Compression stockings are specially designed socks to reduce swelling and improve blood circulation. They are worn during the day but do not need to be kept on for an extremely long period of time (e.g. from breakfast until dinner).
- They have different lengths: above-knee or below-knee. People with thicker calf muscles usually opt for above-knee stockings as it is less tight and uncomfortable on their skin, and different types of compression stockings exert varying levels of pressure on the legs.
- You should consult a doctor to recommend the most suitable stockings for you based on the severity of your varicose veins. [4]
- Elevation of the legs
- Propping the affected legs up on a higher surface will facilitate blood flow from the veins in the legs towards the heart, reducing the amount of blood trapped in the veins.
- Losing weight
- Losing weight will lessen the amount of pressure on the veins. This is not to say that you have to go on a rigorous exercise regime and diet, just that losing any weight might be helpful to lessen the pain caused by varicose veins.
If home treatment proves ineffective and your varicose veins still cause a lot of pain, disrupting your daily routine and your time with loved ones, you may need to see a doctor. They will advise you on procedures available should you wish to opt for them.
How do I know if varicose veins (Singapore) are a cause for concern?
If you are experiencing these symptoms, you should get your varicose veins checked:
- Aching/heaviness in the legs
- Burning, throbbing, cramping or swelling in the lower legs
- Skin discolouration around enlarged, darker veins
- Itching around one or more veins
- Increased pain after not moving legs for a long time
Your doctor will conduct a physical exam and take your medical and family history to determine if and how severe your varicose veins are. You may be required to take an ultrasound scan or an X-ray to confirm the results of the exam, per the doctor’s judgment.
If needed, your doctor may offer you some procedure options:
- Litigation and stripping (surgery)
- This refers to the removal of the varicose vein, or at least the areas which have faulty valves. Two incisions are made in the targeted vein, one at each end of the portion which needs to be removed. The two ends are ligated (tied up) and an instrument is threaded through it; stripping the entire length of the varicose vein. You will be put under general anaesthetic for the operation. [6]
- Laser treatment
- During laser treatment, a high-focus beam of light is aimed at the varicose vein and the extreme heat closes off the vein. Laser treatment can use either external or endovascular (under the skin) lasers, depending on the location of the varicose veins. If an endovascular laser is used, a thin and narrow tube (catheter) is inserted into the vein from a small incision (key-hole surgery).
- Glue treatment
- Depending on the position and the length of vein affected, you may be suitable for varicose vein ablation using medical grade “super-glue” (Cyanoacrylate glue). A fine catheter tube is introduced thru a small incision in the leg and the Cyanoacrylate glue is infused via the catheter into the varicose vein. The vein is sealed close by the glue and disappears after a few weeks.
- Stab avulsion
- Several small incisions are made along the leg, and the varicose vein is pulled out bit by bit through these cuts. Stitches are not needed.
Where should I go?
Most vascular clinics in Singapore should offer treatment for varicose veins. If you are looking for a varicose veins doctor, Singapore Vascular and Interventional Centre is an option for you! Our clinic offers all of the minimally invasive procedures stated above. Feel free to book an appointment with one of our specialists if you are looking for treatment and advice on this condition.
- Tags:
- Causes of varicose veins
- Chronic venous insufficiency
- Early signs of varicose veins
- How varicose veins form
- Leg vein discomfort
- Leg vein problems Singapore
- Poor circulation Singapore
- Singapore vascular care
- Singapore vein disorder guide
- Swollen leg veins Singapore
- Understanding varicose veins
- Varicose vein information Singapore
- Varicose vein prevention tips
- Varicose vein risk factors
- Varicose vein symptoms Singapore
- Varicose Veins Doctor Singapore
- Varicose Veins Singapore
- Vascular issues in legs
- Vein bulging legs Singapore
- Vein health Singapore
- What are varicose veins
