Gangrene refers to the death of tissues in the body due to blockage of blood vessels or infection resulting in insufficient oxygen supply to these tissues.
With gangrene, the aim is to initiate treatment as early as possible, to reduce the amount of tissue damage and loss. Prevention is always better and being aware of how to prevent gangrene is important so that you can avoid the risks posed to your limb and life when gangrene becomes serious. You can find out more about how to prevent gangrene here.
DIAGNOSIS
Gangrene is diagnosed when your tissue turns purplish/black and you lose function and sensation in the affected body part. Certain tests will be conducted when you are diagnosed with gangrene to assess the severity and to guide appropriate treatment.
- Blood tests: Blood is drawn from your arm and tested for signs of infection. For example, an increased count of white blood cells would indicate that bacteria are likely present in the wound. [1]
- Imaging tests: Computerized Tomography (CT) scans, Magnetic Resonance Imaging (MRI) scans and X- ray scans can all be carried out to check for spread of infection to the deeper structures such as the bone and joints. The doctor will also check for gas under your skin as this may be a sign of deadly gas gangrene.
Simultaneously, your doctor will perform a scan on your blood vessels to check for blockages that could be the cause of the gangrene.
- Cultures
- Blood culture: Samples of your blood are drawn and incubated in a warm suitable environment to promote the growth of the bacteria. After the bacteria replicate, it can be identified accurately and tested for appropriate antibiotic susceptibility. [2]
- Tissue/Fluid cultures: Samples of the tissue or the fluid from the affected area is taken and tests are conducted on the samples. This is to determine the specific bacteria responsible for the infection, so that the doctor can prescribe the correct antibiotic to counter the infection. [2]
TREATMENT
After gangrene has damaged the tissue, it cannot be salvaged, but treatment can help to prevent the condition from getting worse.
- Medication: Antibiotics are often administered to treat the bacterial infection. This can either be given via an Intravenous (IV) drip, or taken as tablets. IV drips and injections are usually only necessary if the infection is severe and a more direct form of administration is needed.
- Debridement surgery: This procedure involves thoroughly disinfecting and cleaning the wound, and surgically removing any necrotic (dead) tissue to facilitate better healing. Following this surgery, antibiotics may also be prescribed.
- Maggot therapy: A form of biosurgery, where maggots that have been bred in a sterile and clean environment are used to disinfect the wound. The maggots are placed on the wound and covered up with gauze so that they remain in the wound and out of sight. The maggots feed on the dead tissue and help clean the wound, allowing healthy tissue to then regrow. Risks associated with this treatment are very low, and it has been proven to be an effective treatment for gangrene.
- Angioplasty and Stenting: This is to restore healthy blood flow so that the tissues in the body are receiving the oxygen and nutrients that they need. A tiny balloon is inserted into the blood vessel that is blocked and is inflated to compress the occluding plaque to the side, thus reopening the blood vessel to allow blood to flow normally. A stent (wire mesh tube) may be inserted at the same time to keep the blood vessel open. The restored circulation supports the healing of the wound affected by gangrene.
- Open bypass surgery: In this procedure, a vein or prosthetic graft is used to connect one proximal healthy segment of an artery to another healthy segment more distally, thus bypassing the parts of the blood vessel that are blocked. Blood circulation is restored to the distal tissues thus reducing the risk of gangrene spreading.
- Amputation: In some cases, the patient has no choice but to have an amputation. This occurs when the gangrene is severe and has already affected most of the limb. Debridement surgery is unlikely to help and hence the only way to prevent the spreading of the gangrene is to remove the whole limb. Once the wound heals, the patient can then be fitted with a prosthetic limb and undergo physiotherapy to restore normal movements and daily activities.
After the surgery, your doctor may use a Vacuum-Assisted Closure (VAC) device to further speed up the healing process. Foam dressing is first put into the wound and covered with another layer of plastic film. This film seals the wound and the dressing. A vacuum pump is attached to a tube in the plastic film. As the vacuum pump sucks the air out from under the plastic film, it creates a negative pressure environment at the wound bed, which has been shown to accelerate the growth of healthy tissue.
The VAC also helps to remove excess fluid and exudates from the wound bed, keeping the wound clean and the surrounding skin healthy. The sides of the wound are also drawn closer to each other, thus speeding up the healing of the wound. The setup can be seen in the picture below.
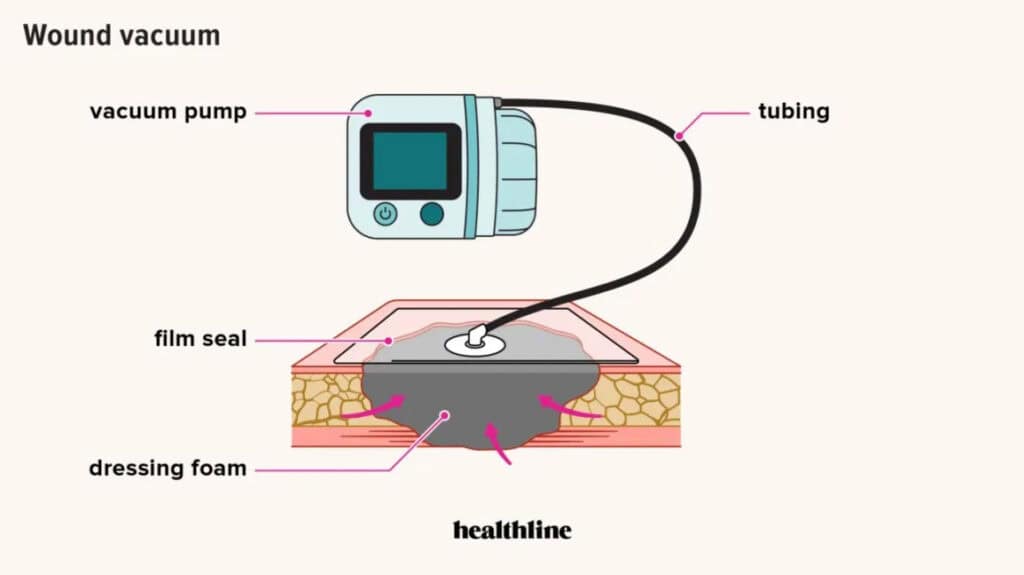
The whole VAC procedure provides an optimal environment for your wound to heal in and will help you to recover from gangrene more quickly.
Should you want to receive treatment for gangrene, feel free to book an appointment with us! Do not hesitate to receive treatment for gangrene as it can be life-threatening if neglected and left untreated. Our doctors will discuss the treatment method that suits your condition, and help you on your journey to recovery, giving you advice on how to prevent gangrene in the future.
Contact details are as follows:
6694 6270 (Call)
9898 3595 (WhatsApp)
en*****@***********tr.com (Email)
6694 6270 (Call)
9898 3595 (WhatsApp)
en*****@***********tr.com (Email)
- Tags:
- Blood flow and gangrene
- Chronic limb gangrene
- Dry vs wet gangrene
- Early signs of gangrene
- Gangrene
- Gangrene amputation risk
- Gangrene diagnosis Singapore
- Gangrene medical emergency
- Gangrene prevention Singapore
- gangrene specialist singapore
- Gangrene treatment Singapore
- Gangrene vascular complications
- Gangrene wound care
- Gangrene wound treatment
- How To Prevent Gangrene
- Infection-related gangrene
- Surgical treatment for gangrene
- Symptoms of gangrene
- Tissue necrosis treatment
- Treating gangrene in Singapore
- Vascular gangrene care
- What is gangrene
