Veins as Vital Pathways in the Circulatory System
The circulatory system is responsible for the transportation of blood throughout the body. Veins act as vessels for blood flow and they serve various purposes:
- Veins act as the return path for blood that has delivered oxygen and nutrients to body tissues. After this exchange occurs in the capillaries, veins carry the oxygen-depleted blood back to the heart and lungs for reoxygenation.
- The contraction of surrounding muscles during movement helps push blood through the veins, especially in the limbs. This movement helps prevent blood from pooling in the lower extremities.
- Veins contain one-way valves that ensure blood flows in the correct direction—toward the heart. This prevents backflow and aids in the efficient return of blood to the heart.
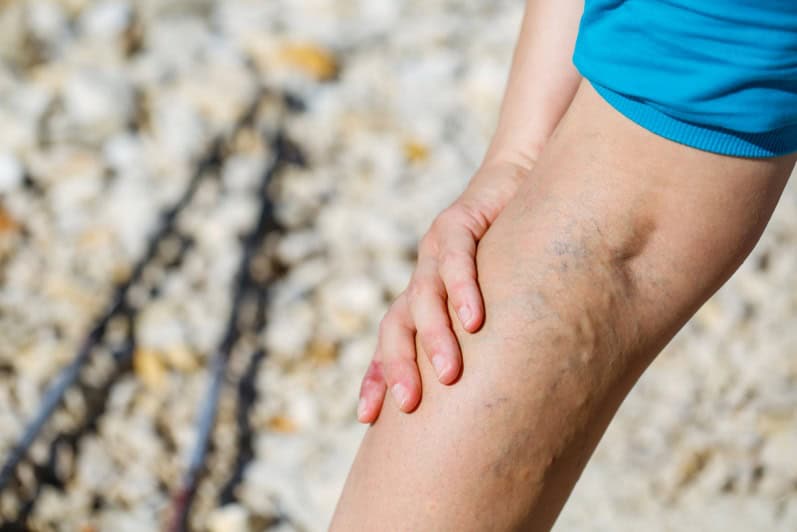
When veins experience dysfunction, as seen in conditions like varicose veins, their importance becomes even more apparent. Varicose veins are enlarged, twisted veins that often result from damaged or weakened vein walls and valves. These conditions can disrupt blood flow, leading to symptoms such as pain, swelling, and discomfort.
Managing varicose veins is crucial not only for symptom relief but also for maintaining the overall health of the circulatory system. Varicose veins can lead to complications like blood clots or skin ulcers. Therefore, addressing varicose veins is not just a matter of cosmetic concern but also one of circulatory health.
(image source: https://cardiacassociatesnj.com/archives/695)
Identifying Common Symptoms & Risk Factors of Varicose Veins
While varicose veins may not always be painful, they are identifiable through certain visual characteristics, such as the presence of dark purple or blue veins that appear twisted and swollen, resembling cords on the legs. However, when varicose veins do cause discomfort, individuals may experience sensations of heaviness or aches in the legs, along with symptoms like burning, throbbing, muscle cramps, and swelling in the lower leg area. These tend to intensify after extended periods of sitting or standing. Itching in the vicinity of the affected veins and alterations in skin pigmentation near varicose veins are also potential signs of this condition.
Understanding and recognizing varicose vein risk factors is vital for both early intervention and preventive measures:
- Age – Increased age contributes to wear and tear of vein valves, leading to blood backflow and pooling.
- Gender – Females are more vulnerable due to hormonal fluctuations during pregnancy, pre-menstruation, or menopause, which relax vein walls.
- Pregnancy – The condition is more likely during pregnancy as the body copes with elevated blood volume to support the growing fetus, causing vein enlargement.
- Family History – A family history of varicose veins raises the risk of developing the condition.
- Obesity – Excess weight places additional pressure on veins, heightening the risk.
- Prolonged Standing – Occupations involving extended periods of standing can strain blood flow, increasing susceptibility to varicose veins.
(image source: https://www.uhhospitals.org/blog/articles/2021/09/varicose-and-spider-veins-whats-the-difference-and-what-to-do)
How Vascular Surgeons Diagnose Varicose Veins
Step 1: Medical Interview
- The vascular surgeon asks about any symptoms you might have, like leg aches, discomfort, swelling, or itching around the veins.
- This assessment helps the vascular surgeon get an initial idea of the problem.
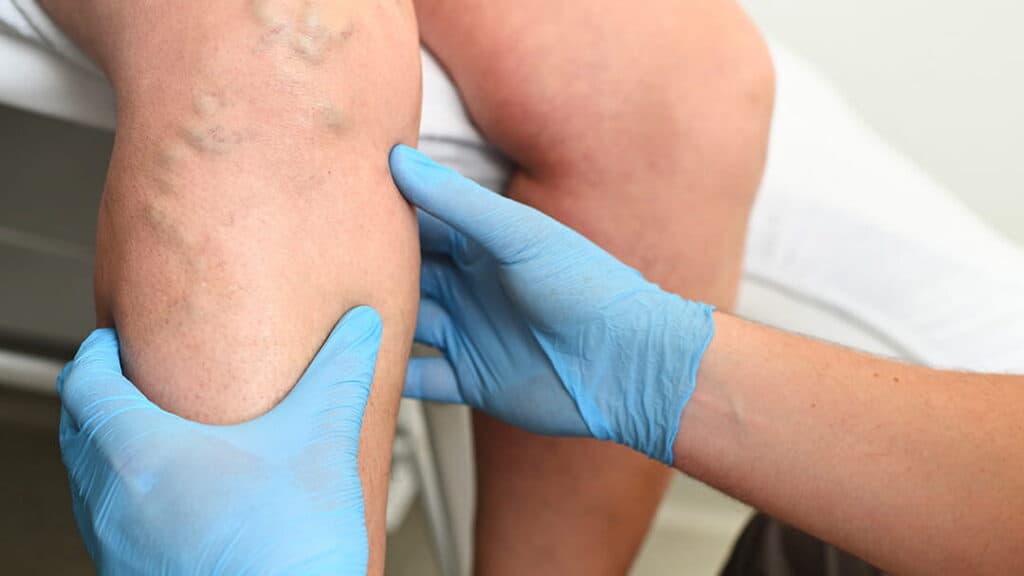
Step 2: Clinical Assessment
- A vascular surgeon examines your legs, and they look for visible signs of varicose veins, such as dark purple or blue twisted veins.
- They assess the size of these veins and check for skin discoloration and texture changes.
Step 3: Ultrasound Scan
- To get a more detailed image of your legs, you may be asked to undergo an ultrasound.
- A technician or sonographer applies a special gel to your legs. An ultrasound transducer is used to emit and receive sound waves. Sound waves bounce off the blood vessels in your legs, creating real-time images on a screen.
- These images confirm the presence of varicose veins. They also reveal critical information about the root causes, such as faulty vein valves or blockages.
Step 4: Comprehensive Diagnosis
- Combining the clinical examination and ultrasound scans ensures a thorough and accurate diagnosis. This comprehensive assessment enables vascular surgeons to develop a treatment plan tailored to your specific condition and needs.
While varicose veins are generally a common and manageable vascular condition, it’s important to be aware of potential complications that can arise. While these occurrences are infrequent, understanding and recognizing these complications is crucial for prompt medical intervention and effective management:
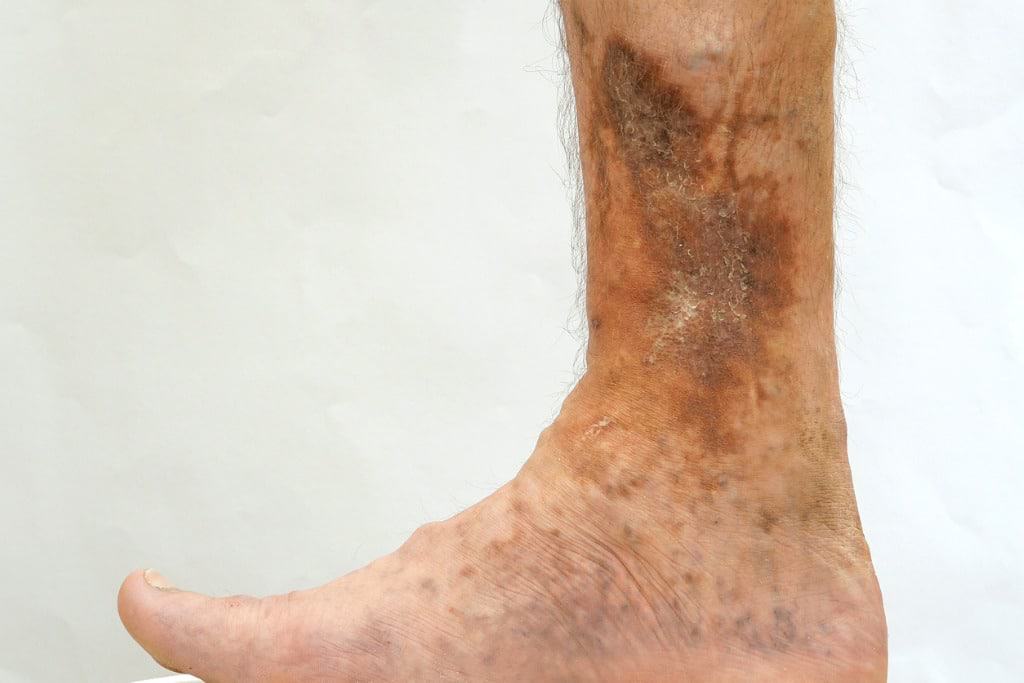
(image source: https://cincyveins.com/conditions/venous-ulcers/)
- Painful ulcers can develop on the skin near varicose veins. Typically, a discolored spot on the skin appears before an ulcer forms. If you suspect you have a leg ulcer, it’s crucial to seek immediate medical attention.
- In some cases, deep veins within the legs may become enlarged, causing leg pain, and swelling. Persistent leg pain or swelling should prompt you to seek medical attention, as it could indicate the presence of a blood clot.
- Occasionally, veins located close to the skin’s surface may burst. While this usually results in minor bleeding, it still necessitates medical attention to address the issue effectively.
Exploring Varicose Vein Treatment Options in Singapore
- Compression stockings improve blood flow within the leg veins, providing relief from associated symptoms, and impeding the progression of the condition. This can effectively boost blood circulation and alleviate discomfort. It’s important to explore alternative treatment options, especially in cases of severe varicose veins.
- Traditional open surgery for varicose veins is commonly referred to as “high-tie ligation and vein stripping.” This procedure necessitates general anesthesia and typically involves an overnight hospital stay. While it has been a conventional approach, open surgery is often associated with several drawbacks. Patients undergoing this method tend to experience higher levels of postoperative pain, and the recovery process can be slower compared to more modern and minimally invasive alternatives.
- Minimally invasive procedures offer similar benefits to traditional surgery but come with reduced pain and faster recovery times. These procedures involve small incisions rather than large openings. Advanced technology allows for tiny punctures through which probes are inserted to seal the affected vein. Typically performed as day surgery, this approach allows for a swift return to daily activities without the need for a prolonged hospital stay. It is conducted under local anesthesia or light sedation, utilizing heat, mechanical, or chemical methods to seal the vein efficiently.
- Radio Frequency Ablation (RFA) – Radiofrequency energy is used to heat up and damage the vein wall. A fast and safe outpatient procedure, it takes about 35-40 minutes to perform.
- Venseal™/VenaBlock Glue Closure – A small amount of specially formulated medical adhesive is used to seal the varicose vein permanently. Through the closure of these veins, blood is rerouted to healthy veins located nearby, providing relief. This procedure provides a comfortable experience and typically is completed within 15-20 minutes.
- Clarivein™ Mechanochemical Ablation – This procedure combines the mechanical destruction of the veins and the injection of sclerosant (a chemical used in sclerotherapy that seals off veins). A special catheter is inserted that has a wire rotating at high speed, damaging the innermost layer of the vein (or the venous intima). At the same time, there is the controlled injection of sclerosant which seals off the vein. This is a painless technique which requires a lot less local anaesthetic injection. Additionally, there is no risk of heat-induced to surrounding nerves due to the mechanochemical ablation technique.
- Cryo-Laser and Cryo-Sclerotherapy (CLaCs) – Suitable for spider veins, this procedure combines transdermal laser and injection sclerotherapy using a chemical sclerosant, all under skin cool (-20C). It leaves minimal scarring and pigmentation post-surgery. This procedure makes use of the Harmony XL PRO. Using its light, laser, and AFT (Advanced Fluorescence Technology), affected blood vessels beneath the skin are targeted.

(image source: https://pharmeasy.in/surgicare/varicose-veins/bangalore)
Selecting the Right Varicose Vein Treatment in Singapore
Choosing the right varicose vein treatment is a decision influenced by several factors, mainly the patient’s individual condition, lifestyle, and the evaluation of an experienced vascular surgeon. Varicose veins are a complex vascular issue, and the most suitable treatment can vary greatly among patients.
Firstly, factors like the severity of varicose veins, and location, and any associated symptoms are key considerations. Mild cases may find relief with non-surgical options like compression stockings, which improve blood circulation and alleviate discomfort. However, as varicose veins progress or become more symptomatic, advanced treatments may become necessary.
Aside from this, the vascular surgeon examines the patient’s lifestyle. Their level of physical activity, occupation, and daily routine can impact treatment preferences. Active individuals or those with physically demanding jobs may prefer minimally invasive procedures for quicker recovery and minimal disruption. Conversely, those leading more sedentary lives may have different treatment preferences.
Preparing for Varicose Vein Treatment
These are three key tips to help you get ready for your varicose vein treatment:
- Before undergoing varicose vein treatment, it’s essential to schedule a consultation with a qualified vascular surgeon. The specialist will evaluate your condition, conduct necessary tests like ultrasound scans, and discuss your medical history.
- Take the time to educate yourself about the varicose vein treatment recommended by your vascular specialist. Understand the procedure’s details, potential risks, and expected outcomes. Ask questions during your consultation to ensure you have a clear grasp of what to expect before, during, and after the treatment.
- Planning for post-treatment recovery is crucial. Depending on the procedure, you may need to arrange for someone to drive you home afterward, especially if anesthesia is involved. Stock up on any recommended compression garments or medications, and ensure your home is set up for a comfortable recovery period. Follow your vascular surgeon’s post-treatment instructions diligently to optimize healing and achieve the best results.
(image source: https://skinvolutionaz.com/how-long-does-it-take-for-varicose-veins-to-disappear-after-laser-treatment/)
Post-Varicose Vein Treatment Expectations & Recovery Tips
- After varicose vein treatment, it’s crucial to understand that immediate results may not be evident. In fact, some patients may experience temporary bruising, swelling, or discomfort. It’s essential to consult with your vascular surgeon to establish realistic expectations and timelines for the full benefits of the treatment to become apparent.
- Adhering to post-treatment instructions is vital for a smooth recovery. This includes taking medications as directed and avoiding activities that may strain the treated area. Make sure to attend all follow-up appointments to monitor your progress and address any concerns promptly.
- To support your recovery and prevent the recurrence of varicose veins, consider adopting a healthy lifestyle. Regular exercise, maintaining a healthy weight, and practicing good vein health habits like elevating your legs when resting can all contribute to long-term success. Staying hydrated and consuming a balanced diet rich in fiber can also help promote optimal circulation and reduce the risk of further vein issues.
FAQs:
Varicose vein treatments are generally safe, but like any medical procedure, they carry some risks. Possible risks include infection, bleeding, bruising, and nerve injury. However, serious complications are rare when performed by a skilled healthcare provider.
During the procedure, you can expect to feel minimal discomfort, and the treatment typically takes a short time. Afterward, there may be some temporary bruising, swelling, or discomfort, but these usually subside within a few days to weeks, depending on the treatment method used.
Preparation often involves discussing your medical history and current medications with your healthcare provider. Depending on the procedure, you may be advised to avoid certain medications or dietary supplements beforehand. Wearing loose, comfortable clothing on the day of treatment and arranging transportation home, especially if you receive sedation, are also common preparations.
After treatment, you can expect to resume most of your regular activities quickly. Your healthcare vascular surgeon will provide post-treatment instructions, which may include avoiding strenuous exercise for a few weeks, and elevating your legs when resting. Follow-up appointments will be scheduled to monitor your progress.
The Vascular & Interventional Centre in Singapore offers minimally invasive treatment for varicose veins. Our vascular surgeons are well-trained in screening, diagnosing, and treating this condition. To find out if the procedure is right for you, you may request a consultation so you can understand your options and choose the best treatment for you. You can contact us at +65 6694 6270 during clinic hours or you can send an e-mail to en*****@***********tr.com.
References:
- https://www.healthline.com/health/varicose-veins
- https://www.sgvascularctr.com/service/vein-diseases-varicose-veins/
- https://www.sgvascularctr.com/wp-content/uploads/2022/01/spider-and-varicose-veins-1.pdf

Dr Chen Min Qi profile
Dr. Chen Min Qi is a fellowship-trained Vascular and Endovascular Surgeon who graduated from the National University of Singapore in 2005. He subsequently completed his basic and advanced training in General and Vascular Surgery while obtaining the Member of Royal College of Surgeons of Edinburgh (MRCSed) qualification in 2010, and the Master of Medicine (General Surgery) qualification in 2015. Dr Chen was subsequently successful at the fellowship exams obtaining the Fellow of Royal College of Surgeons of Edinburgh (FRCSed) qualification in 2016.
Upon completion of his advanced surgical training, Dr Chen Min Qi joined the newly opened Ng Teng Fong General Hospital (NTFGH) as a specialist in the Vascular Surgery division. In 2018, Dr Chen was awarded the Health Manpower Development Plan (HMDP) grant from MOH to undergo further subspeciality Vascular training at the internationally renowned St Mary’s Hospital in London, United Kingdom. There Dr Chen gained further experience in surgeries on complex abdominal and thoracoabdominal aortic aneurysms, redo open repair of abdominal aortic aneurysms following failed EVAR surgeries as well as carotid endarterectomy surgery and lower limb revascularization surgeries.
Upon his return in 2020, Dr Chen Min Qi joined the newly formed Woodlands Health as head of their Vascular service, before joining his current practice at the Vascular and Interventional Centre in January 2023.
- Tags:
- Treatment of varicose veins
- Treatment of varicose veins Singapore
- varicose vein specialist Singapore
- Varicose veins
- Varicose Veins Doctor Singapore
- Varicose veins in legs Singapore
- Varicose veins pregnancy Singapore
- varicose veins procedure singapore
- Varicose Veins Singapore
- Varicose veins surgery
- Varicose veins surgery Singapore
- varicose veins treatment
- varicose veins treatment singapore
